Premature twin journey difficult to put into words - Celebrating Awareness Day
Amour Stewart, local Mother of premature twins, points out that it is hard to condense such an emotional roller coaster of a journey into a story, but she is happy to try and share her experience with us for Prematurity Awareness Day. 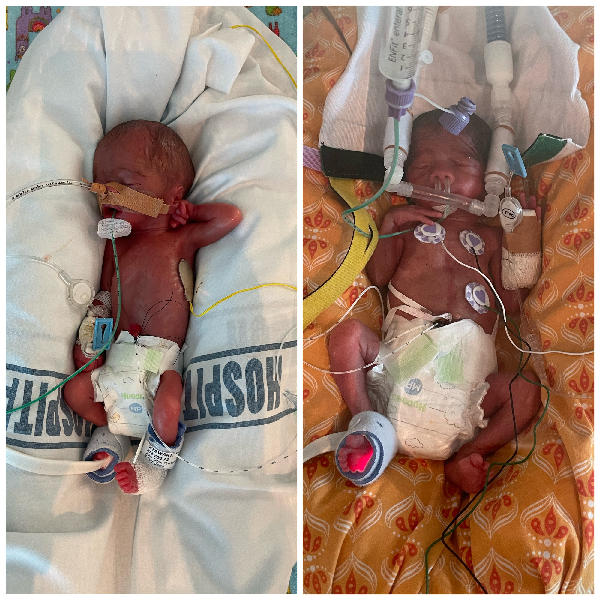
Amour recognised that she would get quite moody when she is pregnant, and this time her overwhelming feelings had given it away.
“Hubby and I had been arguing so he came home from work with a pregnancy test. I took it the next morning. We found out I was pregnant just before he left for work. I was so excited,” she says.
Unfortunately, Amour’s pregnancy experience was not smooth sailing. Before she had tested positive, Amour was starting to get an upset tummy. During her previous pregnancy she had Hyperemesis Gravidarum, a severe form of morning sickness. The symptoms increased as the pregnancy progressed, vomiting every day until 17 weeks.
“They booked a scan to make sure everything was ok because of how sick I was. I remember lying on the bed looking at the screen. As soon as the sonographer put the thing on my tummy, two circles or holes popped up.”
Amour had experienced a couple of miscarriages; one was at 18 weeks in May 2022. When they lost that baby, she had a strong feeling the next time she fell pregnant, that she would have twins.
She was still shocked when twins were confirmed.
“To be honest, now and then I still have a moment where I am like, I made two babies at the same time, I have twins! Who thought I was that responsible?” she giggles.
At the 20 weeks scan they found out they were little boys.
The next scan, at 23 weeks they found out twin one (the baby closest to the exit now known as Waitī), had a low doppler meaning there was not enough blood flow to the placenta. So, he was not growing as well.”
The next chapter began for Amour.
They booked a doppler scan the following week as Waitī hadn’t grown very much.
“The maternal fetal health team in Auckland did a scan and basically said I would be in Auckland till the babies were born. I was injected with my first dose of steroids and told the hospital will ring me once they have my room on the ward.
We booked my husband Shane and 8-year-old daughter into the Ronald McDonald House, and I checked into the maternity ward,” she recalls.
“I spent my time hanging with my family when they’d come up, I’d go with them for a walk to the domain, making friends with my roommates, getting scans, everything seemed to be ok. So, my family went home on day five.”
Day 6, Waitī seemed like he was in distress, so they moved Amour to the delivery suite at about 9am that morning. She sat on a hard narrow bed, in the most uncomfortable position and wasn’t allowed to move because Waitī was so little, and it was hard to pick up his heart rate.
By now Mum was 25 weeks and 4 days gestation.
“I rang Shane to come straight back down to Auckland, it was straight after Cyclone Gabriel had hit. He slept in the chair and was my voice when I felt unheard.”
The next day, Wednesday 12 April, Amour had a doppler scan, nothing had changed, and they booked the big theatre. The nurse put a thick cannula into her tiny vein she remembers uncomfortably, and then pumped it with magnesium.
They got Waitī out at 11:45 am, weighing 490 grams.
Waitā then arrived weighing 690 grams, exactly 200g heavier than Waitī.
Initially Waitī was on continuous positive airway pressure and Waitā was ventilated. 
“They were both so beautiful and precious. I cried when I saw them because they were so little and fragile, and everything was still on the brink of life. The boys went through a lot inside, both having the possibility of having cerebral palsy.
Waitā had a pneumothorax, meaning a collapsed lung. Both needed blood transfusions, the horrid eye tests and X-rays for things like being fed too fast, aspirating, being pumped full of oxygen and vomiting."
“My Waitī was always choosing when to advance to the next stage of breathing, pulling at his continuous positive airway pressure.”
The biggest challenge for Amour, was only being able to see half of her family. It’s draining on your heart, soul and mental health she says, especially as a mother.
“You carry your children in your heart. They make up your heart. It’s like I had two families and two lives. It still triggers me to think about that.”
The boys were in the Special Care Baby Unit (SCBU) for 45 days and the Neonatal Intensive Care Unit (NICU) for 80 days, 125 long days all together.
Every day in the first few weeks the family celebrated each milestone.
“We celebrated them moving breathing levels, moving up nappy sizes, sucking on dummies like they are trying to latch, their eye tests being ok, the times they got to be together, basically we celebrate each day with them because it is special.
But my biggest so far was when my daughter got to hold them for the first time, she was so protective and normally a bit shy, she went to kura the next day and did a big mihi in front of her kura about her baby brothers,” she remembers fondly.
“I also loved when they started breastfeeding, they took to the boob like pros - a proud moment after months of expressing.
“When pregnancy and natural birthing options were taken away from me again because of the emergency caesarean section, breastfeeding was something I wanted to do. I expressed every 2 hours for half an hour for ages.
Everyone said I was pumping too much - but I hadn’t pumped enough with my first girl and our breastfeeding journey was difficult. So, I expressed religiously, crying over missing pump times, it was exhausting. But when it came time to latch and feed, my boys didn’t have to try too hard. and they’ve been mostly breastfed.”
For the most part Amour and the twins had amazing care throughout.
“Most of the nurses showed me extra love and compassion. I remember freaking out at the transition from level 3 care to level 2 care, but those nurses showed us love by cuddling my boys during their tube feeds, making sure they were always warm, comfy, clean and matching.”
In Whangārei it was scary coming from Auckland back to here she says.
“The care is way different, it’s a different pace. It’s a very traumatic transition and something I think both NICU and SCBU should be made aware of, and perhaps spend time in each other's spaces.”
But Whangārei was great she recalls, the nurses do their best under the circumstances.
“They advocate for us and our babies. The nurses and their support team, the health care assistants. They are amazing. They always get us extra food, they gave my family amazing care and tried their hardest to get my babies home.”
She says her advice for anyone going through a premature birth journey is make time to grieve everything you’re feeling. Don’t feel bad if you can’t make it up to your baby every day she says, and to make friends with the other parents.
“It really does lift your morale to talk to other people on the same position,” she points out.
“There’s this part of the journey when you’re forced out into a room with more people and you’ve been in hospital so long, you’re lonely, and you just start talking. You find friends. It makes the journey less lonely and more bearable.”
Last modified:
